Diet Soda: Zero Calories, Not Zero Consequences
What diet soda does to your metabolism
The logic is sound. Sugar drives insulin spikes, promotes fat storage, and contributes to metabolic disease. Removing it while keeping the pleasure of a sweet drink seems like a clean trade. You lose the calories, keep the experience, and move in a healthier direction. That reasoning is not wrong, what it’s missing is what happens after the sweetness hits your tongue.
Your Body Doesn’t Experience Sweetness as a Neutral Event
Tasting something sweet is not passive, it triggers a cascade of biological responses regardless of whether any calories accompany it.
Sweetness signals incoming energy. Your body prepares accordingly. When that energy doesn’t arrive, the mismatch has consequences and those consequences differ significantly depending on which sweetener produced the signal.
Not All Sweeteners Are the Same
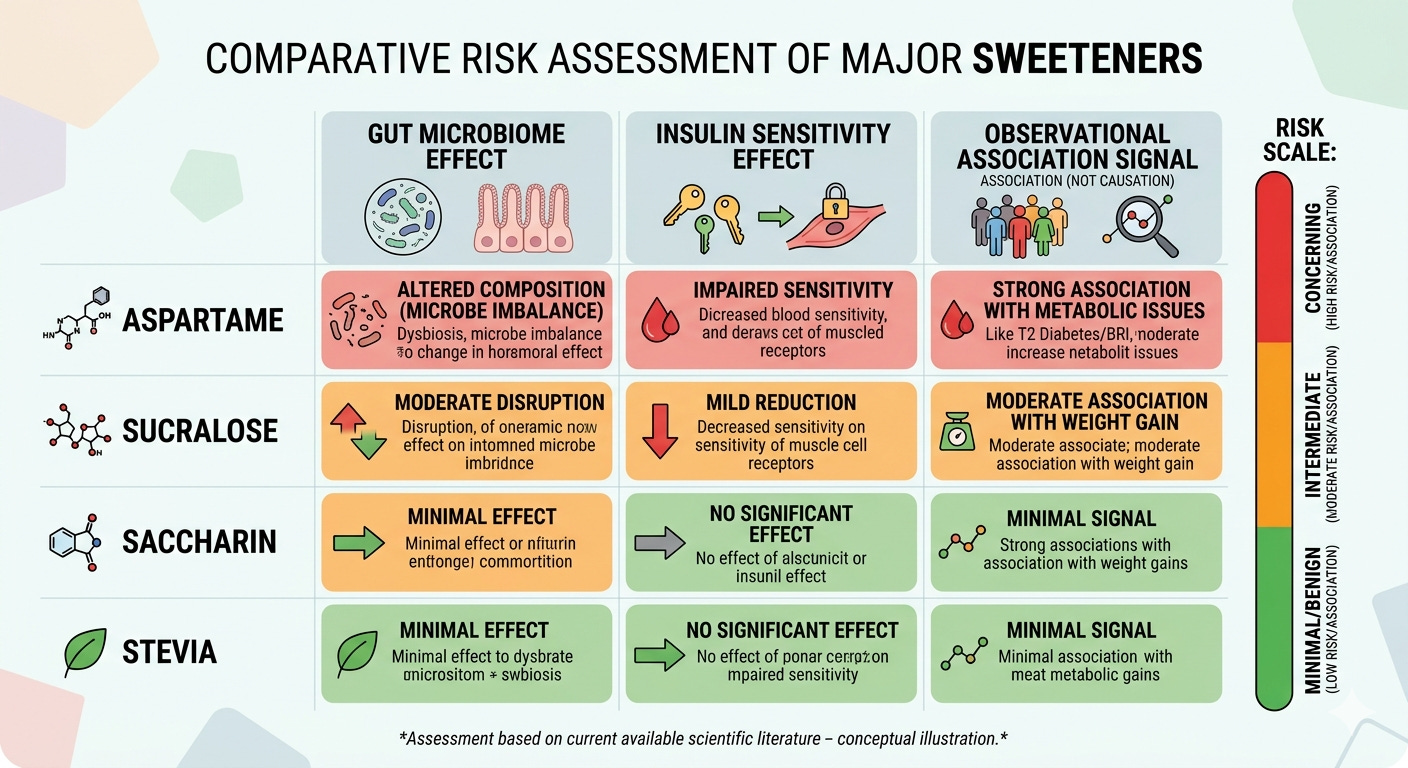
Diet sodas are not sweetened with a single substance. The major non-nutritive sweeteners used commercially, aspartame, sucralose, saccharin, and stevia, have different metabolic profiles.
Aspartame (NutraSweet, Equal) remains the most studied. A 2025 systematic review and meta-analysis by Boxall et al. in the American Journal of Clinical Nutrition, the most comprehensive to date covering 100 experiments, found few effects of aspartame on blood glucose or insulin, either acutely or over medium and long-term follow-up. The certainty of evidence was rated very low across studies, reflecting heterogeneous designs. But among the available sweeteners, aspartame’s metabolic footprint appears limited.
Sucralose (Splenda) is currently the most widely used sweetener in commercially available diet sodas. It is also where the most concerning human evidence is concentrated.
Saccharin (Sweet’N Low) has a well-established gut disruption effect with clinical implications discussed below.
Stevia is derived from a plant and currently shows the most benign profile in the evidence base with important caveats about the size and duration of that evidence base.
If you enjoy evidence-based medical information, subscribe to receive these articles delivered to your mailbox every week.
The Gut Microbiome, Where the Most Important Science Lives
Your gut microbiome is a community of trillions of microorganisms, bacteria, fungi, and other microbes, that colonize your digestive tract. The microbiome plays a central role in how you metabolize food, regulate blood sugar, and respond to insulin.
The landmark study in this area is Suez et al., published in Cell in 2022. In a multi-arm randomized controlled trial of 120 healthy adults, participants were assigned to saccharin, sucralose, aspartame, or stevia at doses below the acceptable daily intake for two weeks. Every sweetener distinctly altered gut and oral microbiome composition but the effects were not equal: saccharin and sucralose significantly impaired glycemic responses, while aspartame and stevia showed less pronounced effects. Mouse experiments confirmed that the glycemic effects were microbiome-mediated; the gut bacteria themselves were the mechanism, not a direct chemical effect of the sweetener.
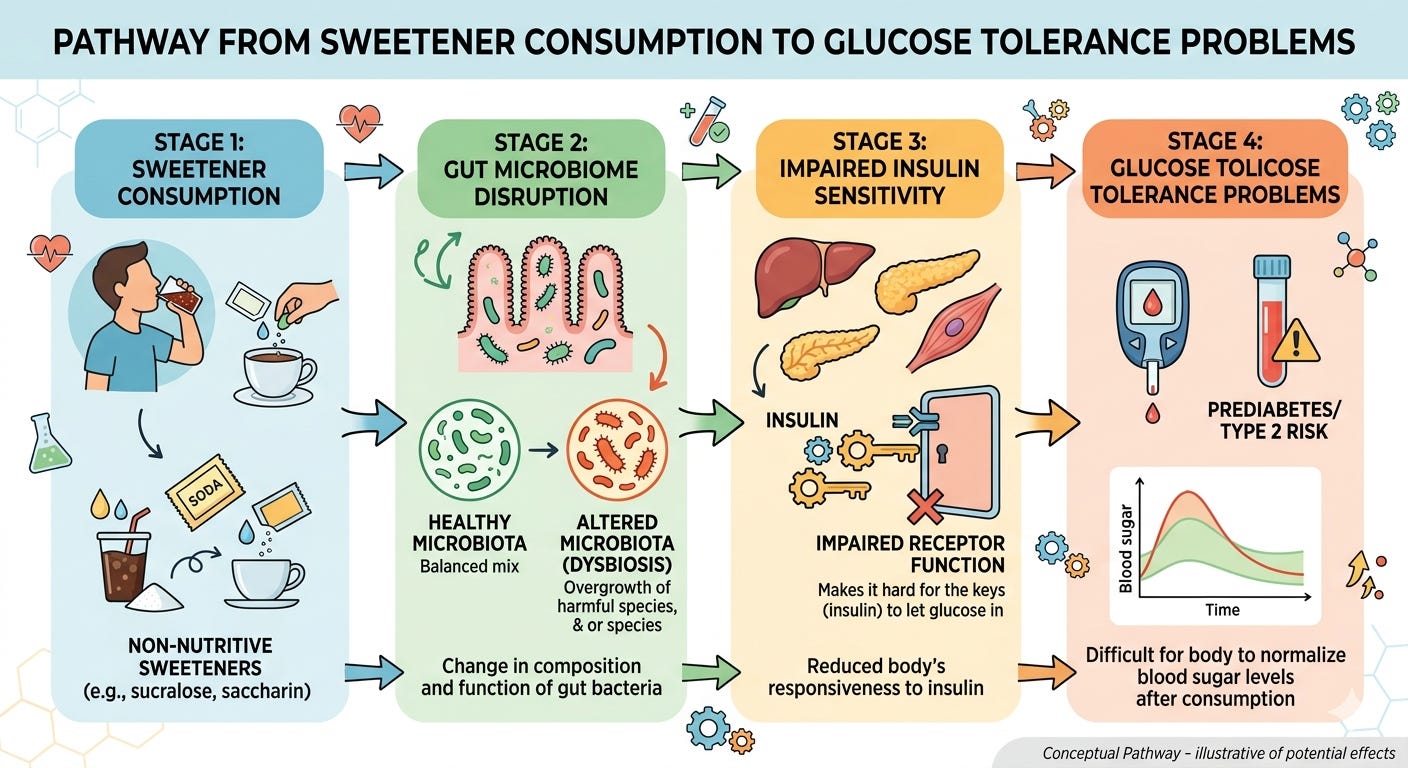
The pathway runs like this: sweetener consumption → altered microbiome composition (dysbiosis) → reduced insulin sensitivity → impaired glucose tolerance. For someone already managing pre-diabetes or metabolic risk this matters.
A 2025 randomized, placebo-controlled, triple-blind trial by Romo-Romo et al. in Clinical Nutrition ESPEN found that 30 days of sucralose consumption at just 30% of the acceptable daily intake produced a 20.3% reduction in insulin sensitivity in healthy lean adults, accompanied by reduced microbial diversity, shifts in bacterial populations, and decreased butyrate, a short-chain fatty acid important for gut health. A separate 10-week open-label RCT by Méndez-García et al. (Microorganisms, 2022) in healthy young adults consuming 48mg of sucralose daily (acceptable daily intake 5 mg/kg daily) found altered gut bacterial abundance and associated changes in glucose and insulin levels on glucose tolerance testing.
The Appetite Question
A separate and more contested question is whether diet soda helps or hinders appetite control over time. The short-term evidence suggests some suppression of sweet cravings. The longer-term picture is less favorable: there is a documented compensation effect, a tendency to offset calorie restriction in one area with increased intake elsewhere, though the evidence here is more heterogeneous than the microbiome data. This is an area where individual variation appears substantial and where the science has not settled.
Why the Research Appears to Contradict Itself
You may have seen headlines claiming diet soda helps with weight loss and headlines claiming the opposite. Both can be drawing on legitimate research. The key is understanding where the difference comes from.
Short-term randomized controlled trials, which replace sugary drinks with diet alternatives under controlled conditions, generally show benefit: lower weight, improved metabolic markers. A 2022 systematic review and meta-analysis by Lee et al. in Diabetes Care, covering 14 prospective cohort studies and 416,830 participants using substitution analysis, found that replacing sugar-sweetened beverages with diet alternatives was associated with lower weight, lower obesity risk, and lower cardiovascular mortality risk.
Long-term observational studies consistently show the opposite: associations with weight gain, metabolic syndrome, and cardiovascular risk. The San Antonio Heart Study (Fowler et al., Physiology & Behavior, 2016) found that daily diet soda users experienced increases in waist circumference nearly four times greater than non-users over a 9.4-year follow-up. This figure has been widely cited and widely criticized, confounding is substantial and reverse causation is plausible (people already struggling metabolically are more likely to switch to diet drinks, making association look like cause). A large cohort study by Buso et al. (Nutrients, 2022) reported a 21% increased risk of obesity per additional 250ml of diet soda consumed daily, with similar confounding caveats.
Where Institutional Science Stands
In May 2023, the World Health Organization issued a conditional recommendation against using non-sugar sweeteners for weight control based on a systematic review finding no long-term benefit in reducing body fat and potential increased risk of type 2 diabetes and cardiovascular disease with prolonged use.
The WHO recommendation has been criticized by nutritionists at Harvard and elsewhere for excluding large substitution studies that showed benefit when diet beverages replace sugary ones.
The Cardiovascular and Renal Risks
An umbrella meta-analysis of 19 meta-analyses published through November 2024 found diet soda consumption associated with approximately an 8% increased risk of cardiovascular disease mortality and 10% increased overall mortality risk. A 2023 systematic review by Gil and Gil in the Journal of Metabolic Health found associations between diet soda and end-stage renal disease and cardiac remodeling in observational data. Causality is not established in either case and confounding is substantial.
A Framework, Not a Verdict
The evidence does not support treating diet soda as categorically harmful. It does not support treating it as metabolically invisible either.
Here is what the science actually justifies: if you are using a diet soda deliberately to reduce your sugar-sweetened beverage intake during a transitional period, the short-term evidence supports that strategy. The problem is not the occasional diet drink. The problem is the chronic daily habit reframed as a health food particularly when the sweetener is sucralose or saccharin and the consumer has existing metabolic vulnerability.
Among the available options, stevia currently shows the least metabolic disruption based on converging evidence from the Suez et al. 2022 trial and a large multi-cohort study of 47,910 adults reviewed by Harrold et al. (PMC, 2024) which found stevia was not associated with obesity risk, unlike sucralose, saccharin, and aspartame which showed positive associations.
Water, unsweetened tea, and sparkling water remain the uncontested options if the goal is metabolic health. If you are going to drink diet soda, knowing what is in it and how the sweeteners differ puts you in a position to make a more intentional choice.
Found this article useful? Share your thoughts. Join the conversation below.
Educational content on The Metabolic Archives is free, because medical information should be accessible to everyone. If you find value and want to support the work, a paid subscription is available and genuinely appreciated. Visit the About Page for additional information.
Disclaimer: The information provided in The Metabolic Archives is for educational and informational purposes only, and is not intended as medical advice, diagnosis, or treatment, and does not constitute a doctor-patient relationship. Do not adopt any recommendation discussed in any article or guides published here, make changes or abandon any prescribed medical treatment without prior consultation with your physician. Always seek the advice of your physician or other qualified health provider for any questions regarding your medical condition and recommended treatment options.
By reading this post, you acknowledge that you have read and agree to the Terms of Service of The Metabolic Archives, which govern all use of this content including restrictions on reproduction.
© 2026 The Metabolic Archives. All rights reserved.



Thank you for this article! Was wondering if there's any "safe" sugar substitutes! Trying to cut back on sweets/sugars, but I like some sweetness to my iced tea! So I'll look for Stevia to use! Thankyou so much!